What is joint protection?
When you’re dealing with joint pain, everyday tasks such as getting in and out of the shower, getting dressed or making the bed can feel like a struggle.
However, you can reduce the pain and strain on your joints by changing the way you do things. This is called joint protection or joint care.
Joint protection doesn’t mean that you should avoid using your joints. It’s simply about using your body in a way that doesn't strain or damage them.
What are the benefits of joint protection?
Research has shown that joint protection can help to reduce pain and make everyday activities easier.
Many people with arthritis also say that they have less stiffness in the morning and fewer flare-ups when they use these techniques regularly. A flare-up, or flare, is a period were your symptoms come back or get worse.
Everyone should look after their joints. But joint care is particularly important for people with arthritis because it can:
What is a joint and how does it work?
A joint is where two or more bones meet and they allow different types of movement.
The joint is held together by a capsule, which stops the bones from moving too far, and inside the capsule, there is an inner lining called the synovium. This makes a thick fluid, known as synovial fluid, that protects the joint.
The ends of the bones are covered with a thin layer of slippery tissue called cartilage. This acts as a protective cushion, stopping the bones from rubbing against each other.
Your muscles are attached to tendons, which are attached to bones. When we move, our muscles pull the tendons, which then pull our bones in certain directions.
Why should I protect my joints?
Arthritis can make daily activities even more challenging. The main obstacles people face are:
- joint pain and aching muscles
- loss of strength
- extreme fatigue, especially at the end of the day
- frustration when everyday tasks take longer to do
- worries about having to rely on other people for help.
However, by taking good care of your joints, you could make everyday tasks a little easier.
How do joints become damaged?
If you have arthritis, your muscles may weaken over time, causing the joint to become unstable. Your bones and cartilage may become damaged, and eventually your joints may change shape.
If you have an inflammatory type of arthritis that causes pain, swelling and stiffness in your joints, such as rheumatoid arthritis, your ligaments supporting the joint capsule can be stretched due to repeated joint swelling.
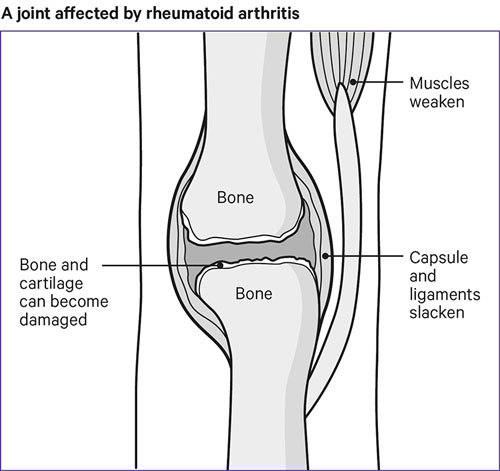
The way you use your joints can contribute to these problems becoming worse, so that’s why joint protection is important.
Your hands are particularly at risk because they have many small joints and are used a lot. You may have problems with activities that need a good grip or co-ordination, such as writing, using your mobile phone, or fastening buttons on clothes.
You may also notice pain and reduced movement of your fingers and thumbs.
When should I start looking after my joints?
We rely on our joints for almost every movement we make. So, it’s best to make joint protection a daily habit.
Even if your joints are already sore, joint protection techniques can help ease the pain. Plus, joint protection can prevent further damage to your joints.
Joint care is a useful skill for any part of the body. But pay special attention to any joints that are affected by arthritis. For instance, if a joint feels painful, weaker or is changing shape.
It may take a little getting used to, but even small changes could make a big difference.
Short-term ways to tackle joint pain and stiffness
There are plenty of ways you can look after your joints. Exercise can keep your joints strong and reduce fatigue and stiffness. Meanwhile, getting a good night’s sleep can help you better manage pain and fatigue.
However, pain can be unpredictable. Some days it might be harder than others to keep moving and that’s okay. Just listen to your body and be kind to yourself.
If you’re having a flare-up or are in severe pain, here are a few ways you might be able to get relief.
Then, when you’re ready, try some of our long-term tips to protect your joints from further damage.
Take painkillers
If you’re experiencing chronic pain, your doctor may prescribe painkillers. There are many different types including:
- Non-opioid painkillers – such as paracetamol.
- Anti-inflammatory drugs – such as ibuprofen or naproxen.
- Compound painkillers – this is when two different drugs are combined into one.
Your doctor will try and find the right painkiller for you depending on your situation and condition. This will help you stay active and keep moving.
Look after your feet
Having sore feet can make it harder to get out of the house. That’s why comfortable shoes are essential.
Wearing good, supportive, properly fitting footwear can help improve your balance and posture. This reduces strain on your joints too.
It’s worth getting your feet measured each time you shop for new footwear. Remember that your feet change shape throughout your life.
If you have long-term feet problems, you might want to talk to your doctor, orthotist or podiatrist. A podiatrist is a healthcare professional who treats foot problems. They can tell you how to best look after your feet and may recommend that you try orthotics. These are insoles, inserts or specially made shoes that are designed to relieve pain and correct changes in your feet.
An orthotist is a healthcare professional who specialises in providing devices, such as splints and insoles, to support weakened joints, reduce pain and improve your mobility. Some devices are made-to-measure.
If you’re on the lookout for footwear recommendations, be sure to check out our online community. Here you’ll find first-hand tips and suggestions from people with arthritis.
Use splints
Wearing splints might offer some relief if you have painful, weak, or swollen joints. There are two types of hand and wrist splints you can choose from – working and resting splints.
If you’re unsure which one is for you, an occupational therapist can explore the options with you. Or you may be referred to a hand therapist. A hand therapist is an occupational therapist or physiotherapist who gives advice on exercises and treatments to improve and maintain the use of the hands.
There are different types of splints including:
- Working splints which provide support to help reduce pain while you’re working or going about your daily activities.
- Resting splints, which are designed to be worn at night if you have pain that affects your sleep or when resting (for example, when watching TV during the day). They have a custom-made cradle with straps to hold it in place.
- Some people find that compression (isotoner) gloves are also helpful in reducing pain and swelling and are easier to wear. These can be worn day or night when working or resting.

Long-term ways to reduce joint pain and stiffness
Painkillers and splints can offer quick relief. But if you really want to prevent further damage and pain, it’s important to keep moving and practise joint protection.
Making these habits isn’t always easy. But even small changes could make everyday tasks such as cooking, cleaning, dressing, and washing a bit easier.
Here are some examples of joint protection:
- Notice any pain you feel and use it as a warning.
- Spread the weight over several joints when carrying things.
- Reduce the effort you put in – labour-saving gadgets can be a great help.
- Avoid gripping things tightly.
- Avoid positions that push your joints into awkward positions as this could lead to further problems.
- Use your joints in more stable positions.
- Stop and think about how you could do something differently if it hurts you.
We’ll dig a bit deeper into these techniques below so that you feel well equipped to try them out.
Respect your pain
Pain is a common symptom for many people with arthritis and it doesn’t always mean that you’re damaging your joints. It can be hard, but it’s important to stay active if you have arthritis because stopping movement could cause more damage to your joints.
However, if you’re in serious pain or feel like your pain is getting worse, it's not something to ignore. It might be a warning sign that you are pushing yourself too far and need to pace yourself or adapt the activity so it’s suitable for you.
Try to notice any aches and pains you may have and take a break every half an hour or so. If you’re still having pain, try taking more breaks next time as it might mean you can keep going for longer.
Many people will give up an activity or a hobby, such as gardening, if it hurts, but it’s better to do a little at a time, with plenty of rest, rather than give up something you enjoy.
Ask yourself: how are you using the joints that hurt the most? Can you think of another way of doing things?
Let’s say your hands hurt when you are making a cup of tea. You could try to pick up the kettle with two hands instead of one. Or, if you’re struggling to stand for long periods, you could try to do some tasks sitting down.
Use stronger joints to do jobs
When carrying items, it’s best to use larger joints where possible because these are protected by stronger muscles.
Try the following tips:
- Use your hip or shoulder instead of your hand to close a drawer or door.
- Hug larger objects close to your body as you carry them.
- Carry bags on your forearms instead of using your hands, as they are less likely to get injured.
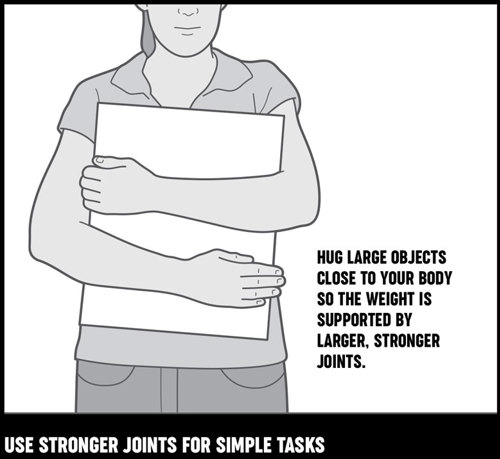
Use stronger joints for simple tasks. Hug large objects close to your body, so the weight is supported by larger, stronger joints.
Spread the load over several joints
If you’re carrying a heavy item, spread the load across several joints. For example, you could use two hands to carry heavy plates. This will put less strain on one joint in particular. The more joints you use to do a job, the better.
Try these tips:
- Use two hands.
- Keep as much of your hand as possible in contact with the object.
- Avoid gripping with your thumbs.
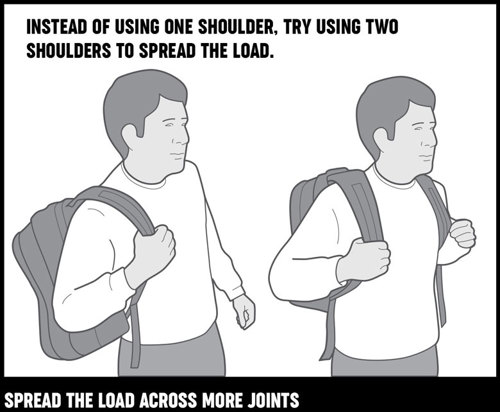
Spread the load across more joints. Instead of using one shoulder, try using two shoulders to spread the load.
Use less effort to do things
Pushing yourself too hard can make your joints more painful. So don’t do too much all at once. Instead, try to make things easier for yourself.
You might want to:
- Ask for help, where possible.
- Reduce the weight of what you lift. For instance, if you’re moving a heavy cardboard box, you could take a few items out before lifting it.
- If you can’t reduce the weight, slide objects along a work surface or use a trolley or wheelbarrow.
- Use labour-saving aids and adaptions to make tasks a bit easier.
Aids are items of equipment that can help you manage everyday tasks such as dressing, cooking and walking. They can include walking aids, easy-to-use kitchen utensils and cutlery with large handles. Adaptations are changes made to your home to help you move around. They can include fixed ramps and baths with built-in handles.
If you’re struggling to do an activity, aids and adaptations could help you to live independently at home. For example, if you’re worried about falls and have been inactive for a while, you might find a walking stick gives you the confidence you need to keep moving.
Many people with arthritis are eligible to have aids and adaptions provided, free of charge, by their local authorities. Your council may call this ‘community equipment’. To see what you’re eligible for, ask your council for a free needs assessment. It varies a lot depending on your needs and where you live. If you’re already seeing an occupational therapist, they will assess your needs and provide you with aids, where needed.
Learn more about gadgets and equipment for your home.

Avoid gripping things tightly
You grip things tightly when doing tasks such as writing, knitting or when using tools like a screwdriver. However, this puts a lot of strain on your knuckle and thumb joints.
To reduce this:
- Take frequent breaks and rest your hands briefly.
- Try to loosen your grip.
- Reduce the length of time you spend doing these activities.
- Use a padded handle to widen your grip.
Avoid positions that might increase your risk of joint problems
Arthritis can damage your joints over time, which can cause your bones and joints to be pushed out of their correct position. This might make everyday tasks - like opening a jar, fastening buttons, or twisting a doorknob - hard, painful, or impossible.
Your hands are most likely to be affected because they have lots of small joints and are constantly used. But certain positions can increase your risk.
For example, you should try to avoid:
- lifting heavy objects with your wrists bent downwards
- using too few joints to do a job, for example, using a few fingers to carry a plastic bag instead of your forearm
- pushing your fingers over towards your little finger and putting pressure on your thumb
- twisting or over-straightening your fingers.
The illustrations below show some examples of tasks that can gradually push your joints into positions that increase your risk, and better positions that you can try. Try them out and see if they help to reduce any uncomfortable or painful feelings in your joints.
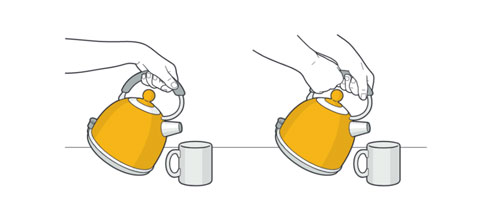
Instead of pouring with one hand, try pouring with two hands.
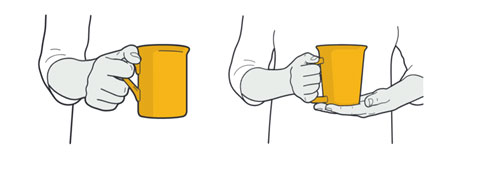
Instead of using a cup with a small, curved handle which pushes your fingers into an awkward position, try using a cup with a larger, straighter handle.
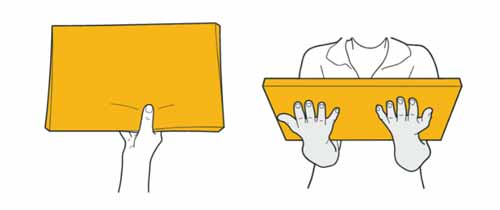
Instead of carrying papers in one hand, try using both hands.
How can I use joints in more stable positions?
Try to use your joints in stable positions that spread the weight evenly over several joints.
Don’t try to push your joints too far. If something is out of reach, for example, then you should get up and move closer to it, rather than stretching into an awkward position.
If you need help, try the following tips:
- Sit or stand as close as you can when working at a table or bench – this reduces stretching and bending.
- Keep your weight supported evenly through both legs, standing with your hips square, and facing forward.
- Use a grip that keeps your wrists straight and your fingers in line with your wrist when carrying things.
- When lifting objects, reduce the strain or pull on your shoulder by keeping your elbow bent and in front of your body, and keeping your palm facing the ceiling when reaching up. To lower your arm, bend your elbow, bringing your hand closer to your body.
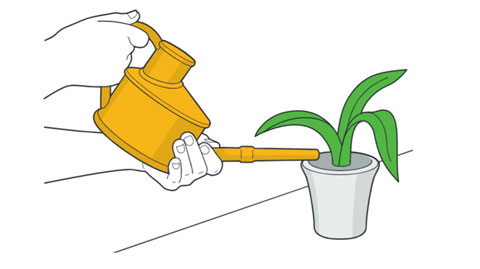
Use more stable positions. Use a grip that keeps your wrist straight and your fingers in line with your forearm.
Making changes
We know it can be hard to change habits. It takes time and patience. But if you stick with it, you might find that your joints become less painful and swollen.
It’s best to make changes bit by bit. You might find it helpful to write down the benefits you’ll get from making the changes. This will remind you why you need to stick with it.
If you find it difficult to make changes, pick a task that’s causing you the most pain and make one change at a time. Even a small change could make a big difference.
If you’re stuck, try the following tips below:
- Work out another way of doing the task which causes less pulling or pain on joints.
- Practise the new movements until you get them right and feel comfortable doing them.
- Keep practising until the new movements become automatic and second nature.
Joint care at work
You should try and make joint protection a habit, even when you’re at work.
Sitting down all day isn’t good for you, so if you work at a computer, try to take a break and stand up every 30 minutes or so. Better yet, go for a short walk if you can. This will allow you to stretch your legs and arms to prevent them from becoming stiff.
It’s also worth making sure that your work surfaces are the correct height. That way, you don’t have to stoop or stretch to work. If you’re sitting, think about whether your seat is comfortable, supportive and at the right height and depth for you. Your chair should be adjusted so your hips and knees are at right angles, and you should have good support for your lower back. Remember to keep your wrists relaxed if you are typing too.
If you have to stand for long periods or work in a cramped position, it might leave you feeling tired or achy. If this is the case, it might be worth seeing if there are any tasks you can do sitting down.
Getting joint care support at work
Living with arthritis or joint pain might make your working life harder. But you have options and rights and it’s important that you understand them.
In some cases, your employer might be required to make reasonable adjustments for you at work. For instance, they might change your work hours or provide you with special equipment that helps to protect your joints.
If you need advice on adjustments at work, you and your manager can arrange an assessment. An occupational therapist or a Disability Employment Advisor (DEA) can do this too.
An occupational therapist is trained to help improve your ability to do everyday tasks. They can also recommend useful equipment specially designed for your condition. If you haven’t told your employer that you have arthritis, an occupational therapist can also give you advice about changes you could make yourself.
Both an occupational therapist and a DEA can advise you on how to improve the way you work. Plus, they can show you equipment that may help you do your job more easily.
You can contact a DEA through your local Jobcentre Plus office. If necessary, a DEA can also help you retrain for more suitable work. You could also get support from the Access to Work Scheme.
Will exercise help my joint pain?
Many people with arthritis worry that exercise could further damage their joints. But, the truth is, exercising is good for us.
Not only does it reduce symptoms such as pain and fatigue, but it’s great for your mental health too.
If you're new to exercise and don’t know where to start, it's a good idea to start slowly and build up gradually. If you’re feeling anxious, talk to your doctor or try a low-impact activity such as walking, cycling, tai chi or yoga.
Remember that any activity is better than nothing. Your body is designed to move and resting too much could actually harm your joints and the tissues around them.
Many exercises don’t require special equipment. It’s all about finding what works for you. If you find an exercise you enjoy, chances are you’ll stick with it and stay active.
Some people find it motivating to exercise with a friend or in a group. We run activities across the country, such as walking groups and chair chi, for instance.
What can I do to improve my grip?
Many people with hand arthritis find their grip becomes weaker and their hands become stiffer. This can be very frustrating. But regular hand exercises can improve your grip.
Practise them daily for short periods a few times a day. Start slowly and build up the amount of exercise you do over several weeks. Find what works for you and adapt the exercises to suit your needs. If your hand is painful, you could use warm water and a sponge to soothe any sore or achy joints.
Ask to be referred to an occupational therapist, physiotherapist, or hand therapist if you want more exercises to suit your needs.
A physiotherapist, for example, helps people with an injury or long-term health condition be active and independent. They’ll offer movements, exercises, manual therapy, education and advice to help ease your pain and move your muscles and joints more easily.
How to manage fatigue
Fatigue isn’t the same as tiredness. It’s extreme mental and physical exhaustion that doesn’t improve with rest or sleep.
It’s unsurprising that many people with arthritis feel fatigued. Living in constant joint pain can wear you down. Many arthritis medicines can make you feel sleepy. Plus, sleep disturbance and low mood can make you feel exhausted.
Fatigue is an invisible symptom, but it can be debilitating and affect your day-to-day life. However, you can help make your energy last a bit longer by:
- practising joint protection
- pacing yourself and avoiding the ‘boom-and-bust' cycle — this is when you might do too much on one day and feel unable to do anything the next
- planning and setting priorities - you might find it helpful to use a calendar
- finding a less tiring position to do activities in
- becoming better organised
- taking time to rest throughout the day
- practising relaxation techniques, such as meditation or deep breathing.
How will a healthy diet help my joints?
It’s important to eat a healthy, balanced diet if you have arthritis. This will give you all the nutrients you need such as calcium, vitamin D and iron.
Plus, it’ll help you maintain a healthy weight. Being overweight puts an extra burden on the joints in your knees, hips ankles and feet, causing pain and mobility problems.
Your plate should include a variety of foods from all five food groups. This includes:
- fruit and vegetables
- potatoes, bread, rice, pasta and other starchy carbohydrates
- beans, pulses, fish, eggs, meat and other proteins
- dairy and alternatives
- oils and spreads.
Eating a Mediterranean-style diet is a good option, because it is packed with lots of fruit and vegetables, oily fish, nuts, seeds, and olive oil.
Some people take dietary supplements to help protect their joints. Research results are mixed though, so if you decide to try supplements, you should question what they’re doing for you. Then decide if you want to continue taking them depending on whether you notice any improvement.
Who else can provide help and support?
If you’re struggling to look after your joints, remember that you’re not alone. There are healthcare professionals, local groups, and friends and family who can all help to provide support and encouragement.
Healthcare professionals
If you need a helping hand with joint care, many healthcare professionals who can give you advice. These include:
Joint protection programmes
Because changing the habits of a lifetime can be very difficult to do, many people find it helpful to get together with others who wish to do the same.
Many occupational therapy departments offer joint protection programmes, where you can learn more about joint protection and swap tips with other people.
If you find the self-help methods suggested here useful, you may like to join a local group.
The National Rheumatoid Arthritis Society (NRAS) also run a programme for people with rheumatoid arthritis. There are similar programmes available locally for people with long-term medical conditions like arthritis.
Be sure to ask your doctor’s surgery or rheumatology unit about the NHS Expert Patient Programme too.
Look at our services and support information to check if we run a group in your area.
Family and carers
Learning about joint protection may help your family and carers better understand some of the problems people with arthritis face. Some people find it very helpful to get their family or friends involved as they practise some of the ideas mentioned on this page.
You may find that it’s easier to make joint protection a habit if you have support and feedback.
Yvonne’s story
 With hindsight, I am sure my symptoms began in my early 20s. I was working as a teacher, but my symptoms kept gradually getting worse over the years. I had pain everywhere, I was stiff, I was aching, and I was muddled. By 45, I was finding teaching difficult, so I went to the GP for help. Sadly, I never went back into the classroom again.
With hindsight, I am sure my symptoms began in my early 20s. I was working as a teacher, but my symptoms kept gradually getting worse over the years. I had pain everywhere, I was stiff, I was aching, and I was muddled. By 45, I was finding teaching difficult, so I went to the GP for help. Sadly, I never went back into the classroom again.
It turned out that I had osteoarthritis in most of my joints, Raynaud’s phenomenon and fibromyalgia. Later, I also developed Sjogren’s syndrome.
When I took time out of the classroom, my pain levels soared. I kept a pain diary. It hurt to get out of bed, it hurt to stay in bed. It was just an awful time for me. Then my GP signed me onto a course, and it was my turning point.
I realised I wasn’t alone. Lots of people in all age groups were just like me. It was like magic. This was where I learnt about aids, pacing and adapting and accepting help from people. Now, using joint protection, I could keep my joints as healthy as possible.
For me, joint protection is about making sure you use your body properly, so posture is important. It’s about lifting things safely. For instance, I often ‘cuddle’ things to get them from one place to another, like my milk container.
I don’t buy a 6-pint of milk because that’s too heavy and I also use a kettle tipper. The kettle is secured in a ‘cradle’ that can tip without me having to carry it.
I love gardening too. To make sure I pace myself, I listen to a podcast and only work for the length of the podcast. Then I stop or change to a task that uses my body differently. I also use splints to help my wrists stay safe and I have a box on wheels, which I can sit on while I work.
I’ve also adapted how I garden. Over time, we have built some raised beds. They are up to my knee height so I can sit on them.
Physical activity is so important too. I stay active by being in the garden, going out, tackling housework and being with my grandchildren. But I also do exercises that strengthen my knees, hips and shoulders.
I have a routine that I follow closely. After doing these exercises for two weeks I started to feel the difference and I notice it when I skip them. Twenty years on from that desperate time, I feel great. I only have one joint replacement, I’m sure that the exercise has kept the joints going longer.
I’d say that if you are new to joint protection, don’t try to do a million things at once. Just choose one thing you want to be able to do.
Then remember there are lots of people who have already tackled this problem – you don’t have to do it all yourself.
Ask around for ideas, use the internet, use health professionals and people like your occupational therapist. Take your time and then go for it.