What is arthritis?
The word arthritis is used to describe pain, swelling and stiffness in a joint or joints. Arthritis isn’t a single condition and there are several different types.
Around 10 million people in the UK are thought to have arthritis. It can affect people of all ages – even children and teenagers. Some forms of arthritis are more common in older people.
If you have pain in or around a joint or joints that doesn’t go away after a few days, you should see a doctor. Finding out what’s causing your pain is key to finding the right treatment and self-help options.
Although there’s no cure for arthritis, treatments have improved greatly in recent years and, for many types of arthritis, particularly inflammatory arthritis, there’s a clear benefit in starting treatment at an early stage.
It may be difficult to say what has caused your arthritis. There are several factors that can increase the risk of each type of arthritis. It could be that the genes you inherited from your parents or grandparents made you more likely to get arthritis.
Arthritis can make life tough by causing pain and making it harder to get about. The symptoms of arthritis can vary from week to week, and even from day to day. Many types, such as osteoarthritis and rheumatoid arthritis, are long-term conditions.
However, with the right treatment and approach you can manage your symptoms.
Whatever condition you have, remaining physically active will help you stay mobile and will be good for your general health.
What is a joint and how does it work?
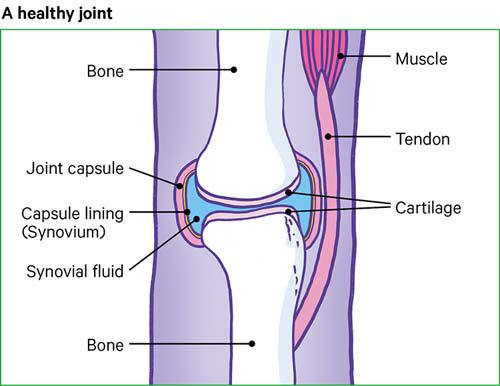
A joint is where two or more bones meet, such as in the fingers, knees, and shoulders. Joints hold bones in place and allow them to move freely within limits.
Most of the joints in our body are surrounded by a strong capsule. The capsule is filled with a thick fluid that helps to lubricate the joint. These capsules hold our bones in place. They do this with the help of ligaments. These are a bit like very strong elastic bands.
The ends of the bones within a joint are lined with cartilage. This is a smooth but tough layer of tissue that allows bones to glide over one another as you move.
If we want to move a bone, our brain gives a signal to the muscle, which then pulls a tendon, and this is attached to the bone. Muscles therefore have an important role in supporting a joint.
Main types
Because there are several types of arthritis, it’s important to know which one you have. There are some similarities between these conditions, but there are also some key differences.
Osteoarthritis
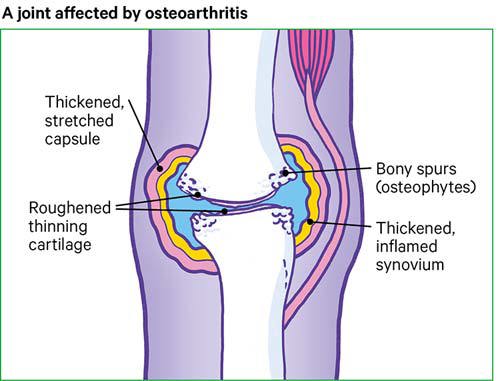
The most common type of arthritis is osteoarthritis. It is estimated that around 8.75 million people in the UK have seen a doctor about osteoarthritis.
Osteoarthritis starts with the roughening of cartilage.
If this happens, the body can put in place a ‘repair’ process to try to make up for the loss of this important substance. The following can then happen:
- Tiny bits of extra bone, called osteophytes, can grow at the ends of a bone within a joint.
- There can be an increase in the amount of thick fluid inside the joint.
- The joint capsule can stretch, and the joint may lose its shape.
Sometimes, the early stages of osteoarthritis can happen without causing much pain or trouble. However, it can lead to damage inside a joint, as well as pain and stiffness.
Osteoarthritis is more common in women and usually affects people from the age of 45 onwards. The parts of the body most commonly affected are the knees, hands, hips, and back.
Keeping active will help you maintain a healthy weight, and this will reduce the pressure on your joints. Doing regular exercise will keep muscles around a joint strong, and this will help to support and stabilise a joint affected by osteoarthritis.
Being overweight can make you more likely to get osteoarthritis and can make it worse.
Taking painkillers, such as paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen can help reduce your symptoms and allow you to stay active. Keeping active will also reduce pain, stiffness and swelling.
There are NSAID creams that you can rub into the affected area. It might be an idea to try these first.
There is a range of pain relief options available. If you’re finding the pain of osteoarthritis difficult to cope with, a doctor or physiotherapist would be able to give you specific advice.
If your osteoarthritis becomes severe, particularly in your knees and hips, your doctor might discuss with you the possibility of surgery. This is usually considered only after you’ve tried all the other treatment options.
Joint replacements are now very sophisticated and successful.
Gout and calcium crystal diseases
Gout is a type of inflammatory arthritis that can cause painful swelling in joints. It typically affects the big toe, but it can also affect other joints in the body.
Joints affected by gout can become red and hot. The skin may also look shiny and can peel.
It’s caused by having too much urate, otherwise known as uric acid, in the body. We all have a certain amount of urate in our body.
However, being overweight or eating and drinking too much of certain types of food and alcoholic drinks can cause some people to have more urate in their bodies. The genes you inherit can make you more likely to develop gout.
If it reaches a high level, urate can form into crystals that remain in and around the joint. They can be there for a while without causing any problems and even without the person realising they are there.
A knock to a part of the body or having a fever can lead to the crystals falling into the soft part of the joint. This will cause pain and swelling.
There are drugs that can reduce the amount of urate in the body and prevent gout attacks. Examples are allopurinol and febuxostat. If you’re having a gout attack, you’ll also need short-term pain relief. Non-steroidal anti-inflammatory drugs (NSAIDs) as well as paracetamol can be good drugs to try first.
Men can get gout from their mid-20s, and in women it’s more common after the menopause. Taking water tablets can increase the risk of gout.
There are also conditions that cause calcium crystals to form in and around joints.
We all need calcium to make bones and teeth strong. However, some people can have too much calcium in their bodies, which can then form as crystals around joints. This can lead to painful swelling.
Calcium crystal diseases tend to clear up on their own. Taking painkillers and NSAIDs, and applying an ice pack wrapped in a damp towel, can soothe the pain and swelling.
Rheumatoid arthritis
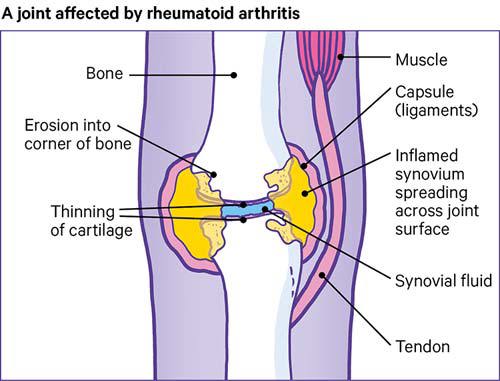
Rheumatoid arthritis is a type of inflammatory arthritis. It is what is known as an auto-immune condition.
The immune system is the body’s natural self-defence system, and it protects us from infections and illness. When someone has an auto-immune condition, the body’s immune system mistakenly attacks the body’s healthy tissues, such as the joints, causing inflammation.
Inflammation is normally an important tool in the immune system. It occurs when the body sends extra blood and fluid to an area to fight an infection. This is what is happening for example if you have a cut that gets infected, and the skin around it becomes swollen and a different colour.
However, in rheumatoid arthritis the inflammation and extra fluid in a joint can cause the following problems:
- It can make moving the joint difficult and painful.
- Chemicals in the fluid can damage the bone and joint.
- The extra fluid can stretch the joint capsule. Whenever a joint capsule is stretched, it never quite returns to its original position.
- Chemicals in the fluid can irritate nerve endings, which can be painful.
As well as causing pain and stiffness, inflammation can cause permanent damage to a joint. Starting effective treatment early on can help to minimise damage.
Symptoms of rheumatoid arthritis can include:
- swollen and tender joints
- swelling and stiffness in joints in the morning that lasts for longer than half an hour
- severe tiredness, also called fatigue
- a general feeling of being unwell.
Rheumatoid arthritis often starts in the small joints of the hands and feet, and it can affect the same joints on both sides of the body at the same time. It can start quite slowly and then gradually get worse, or it can start more aggressively.
Rheumatoid arthritis can affect adults of any age. It most commonly starts among people between the ages of 40 and 60. It’s more common in women than men.
There are drugs that can slow down an over-active immune system and therefore reduce the pain and swelling in joints. These are called disease-modifying anti-rheumatic drugs (DMARDs) and include biological therapies.
If you have rheumatoid arthritis, treatment will start with conventional DMARDs. These can have the overall effect of reducing the activity of your immune system, which is overactive and causing damage to your body.
If these drugs have been tried and don’t work, doctors will look at the possibility of trying the newer biological therapies. Biological therapies have a more targeted effect on the immune system.
Spondyloarthritis
Spondyloarthritis is a word used to describe a number of conditions that cause pain and swelling, mainly around the joints of the spine.
In these conditions there is inflammation of small pieces of connective tissues, called entheses. These are tough little cords that join either ligaments or tendons to bones.
Ankylosing spondylitis
Ankylosing spondylitis is a type of spondyloarthritis and it causes pain and swelling, mainly around the joints of the spine.
In this condition, in response to inflammation around the spine, the body can create more of the mineral calcium. This mineral is normally used by the body to make bones strong. However, in ankylosing spondylitis the extra calcium can make new bits of bone grow in the spine, and this will cause pain and stiffness.
This condition typically causes pain in the second half of the night, and swelling of your back in the morning that lasts for more than half an hour.
There are drugs that can slow this process down. Keeping active will help to minimise stiffening of the spine, while maintaining a good posture will help prevent increased curving of the spine.
Ankylosing spondylitis usually occurs between the ages of 20 and 30. It is more common among men.
Psoriatic arthritis
Psoriatic arthritis is an auto-immune condition. It is also a type of spondyloarthritis.
The body’s immune system can cause painful swelling and stiffness within and around joints, as well as a red scaly skin rash called psoriasis. The rash can affect several places in the body, including the elbows, knees, back, buttocks and scalp.
It is also common to have severe tiredness, otherwise known as fatigue.
Disease modifying anti-rheumatic drugs (DMARDs) and biological therapies can treat the cause of the inflammation in joints. There is also a variety of treatments, such as creams and medications, for psoriasis.
Psoriatic arthritis usually affects people who already have psoriasis. However, some people develop the arthritis before the psoriasis. It’s possible to have the arthritis but no psoriasis at all.
This condition can affect people of any age, but tends to affect adults.
Juvenile idiopathic arthritis (JIA)
If someone is diagnosed with inflammatory arthritis before their sixteenth birthday, it’s called juvenile idiopathic arthritis, or JIA.
There are different types of JIA. They are auto-immune conditions, and the immune system can cause pain and swelling in joints.
The earlier someone is diagnosed with JIA, the better. This is so that effective treatment can be started and limit any damage to the body.
There are drugs that can treat the symptoms, such as painkillers and non-steroidal anti-inflammatory drugs (NSAIDs). Disease-modifying anti-rheumatic drugs (DMARDs) and biological therapies can slow down or stop the arthritis causing the swelling inside the body.
There are about 12,000 young people in the UK who have JIA.
Should I see a doctor?
It’s common to have aches and pains in your muscles and joints from time to time. This may especially be true if you take part in unusual or strenuous physical activities.
So, how can you tell the difference between the early signs of arthritis and normal pain and stiffness? And, how do you know when you should see a doctor about your symptoms?
If you have swelling or stiffness that you can’t explain and that doesn't go away in a few days, or if it becomes painful to touch your joints, you should see a doctor. The earlier you get a diagnosis and start the right type of treatment, the better the outcome will be.
Here are some other things to think about that might help you decide whether you need to see a doctor:
Persistence of symptoms
- How and when did the pain start?
- If the pain came on after unusual exercise or activity you may have just overdone it a bit, and the pain should ease within a few days.
- See a doctor if the pain isn’t linked to an injury or if the pain won’t go away.
Swelling of joints
- If a joint becomes swollen, and isn’t linked to an injury, you should see a doctor.
- This is especially important if you’re also unwell or have a fever, or if the joint is red and warm.
Effects on your daily life
- See a doctor or other relevant healthcare professional if you’re unable to do everyday tasks due to joint or muscle pain.
- If you’ve lifted something heavy and hurt your back, for example, take some painkillers, apply some heat and try to stay active. If the pain doesn’t ease after a couple of weeks or so, see a doctor.
It’s important to see a doctor if you get any new symptoms or if you have any trouble with drugs you’re taking.
If you have an appointment with a doctor, to help make sure you get the most out of it, you could take a list of questions with you and tick them off as they are discussed.
You could also keep a symptoms diary with details of how you’re feeling in between appointments. Some people find that taking a friend or relative with them to an appointment can provide support and ensure that all important points are discussed.
Other conditions that have similar symptoms to arthritis
There are a number of other conditions that can cause pain and possibly swelling in and around joints.
Lupus
Lupus is an auto-immune condition. The immune system mistakenly attacks the body’s own healthy tissues.
There can be many symptoms of lupus. It’s possible for the heart, lungs and other organs of the body to be affected.
Joint pain and swelling is common in lupus, particularly in the small joints of the hands and feet. Joint pain in lupus can move around from one joint to another.
Lupus can be difficult to diagnose, as it can cause many different symptoms which often appear like other conditions.
Fibromyalgia
Fibromyalgia is a long-term condition that can cause pain and tenderness all over the body.
Symptoms can be similar to arthritis. However, the symptoms are mainly in the muscles rather than the joints.
The most common symptoms of fibromyalgia are:
- widespread pain
- trouble sleeping
- when you do get sleep, it can be unrefreshing
- fatigue
- headaches
- difficulty concentrating
- a poor memory.
If you have fibromyalgia, you’re probably very sensitive to pain or physical pressure.
Polymyalgia rheumatica (PMR)
Polymyalgia rheumatica (PMR) is a condition involving painful and stiff muscles. The hips, shoulders and thighs are commonly affected.
Lifting both arms above your head can be painful and difficult. The pain and stiffness are often worse in mornings. Other symptoms include a general feeling of being unwell and fatigue.
It mainly affects people over the age of 70.
Some people who have polymyalgia rheumatica develop a condition called giant cell arteritis (GCA). This affects the blood vessels in the head and can lead to symptoms of pain and tenderness around the side of the head.
Giant cell arteritis can also cause pain in the tongue or jaw when chewing, and in rare cases problems with vision or even loss of vision. If you get any of these symptoms, it’s important to see a doctor urgently. If left untreated, giant cell arteritis can lead to permanent damage to eyesight, even blindness.
Both polymyalgia rheumatica and giant cell arteritis can be treated effectively with steroids, normally tablets.
Back pain
Back pain is a common problem that affects many of us. It’s usually caused by a simple muscle or ligament strain and not usually by a serious problem. There might not even be a specific cause.
Back pain will usually clear away in a couple of weeks.
Remaining active while taking painkillers is often the best thing you can do.
Tendinopathy
Tendinopathy is a condition in which tendons, the strong cords that attach muscles to bones, are painful.
The affected part of the body may be hot, swollen and red. This can make moving that part of the body difficult. You might also feel a grating sensation.
This can be caused by over-use of that part of the body. Stopping or altering the activity that caused the problem may be the first step to recovery.
Remaining generally active and taking painkillers can also help.
Applying an ice pack, such as a bag of frozen peas wrapped in a tea towel, can also reduce pain and swelling.
Information related to other conditions
Managing symptoms
As well as medical treatments, there are many things you can do to help yourself manage your arthritis.
You might not always feel like exercising if you have arthritis. And you might be worried that exercising will make your pain or your condition worse.
However, exercise can make symptoms such as pain and swelling better. There are several reasons why this is the case:
- Your muscles will become stronger. This will provide better support to the joint.
- Your joints will become supple and less likely to become stiff.
- Your joints will be able to maintain their range of movement.
- Exercise improves your overall health and fitness and can help you maintain a healthy weight.
- Exercise leads to the release of chemicals in the body called endorphins. These are painkillers produced naturally by the body. Releasing them into the blood through exercise can make you feel good.
- Exercising regularly can help you get good sleep, which can help the body repair itself.
Type of exercise
People usually find that low-impact exercise is best. Swimming, cycling, brisk walking, yoga, T’ai Chi, and Pilates are all examples of exercises that have helped people with arthritis. It’s good to find something you enjoy so that you keep doing it.
You may feel some discomfort and sometimes pain when you exercise. This feeling is normal and should calm down a few minutes after you finish. It’s not a sign that you are hurting yourself. Exercise will help reduce pain and can help you manage your arthritis better.
While you can push yourself and do strenuous exercise, it’s important not to overdo it. If you are in pain that you can’t cope with during or after your activity, you will need to see a doctor. The key is to start off gently and to gradually increase the amount you do.
Regular exercise is also an important part of maintaining a healthy weight. This will improve your symptoms as it will take pressure off joints. Being overweight can make someone more likely to have inflammation in their body.
The best way to lose weight is to have a healthy, low-fat, low-sugar and balanced diet. Make sure you have plenty of fresh fruit and vegetables, drink plenty of water, and exercise regularly. If you burn off more calories than you consume on a daily basis, you will lose weight.
If you are ever struggling and need support or motivation to keep active, see a GP or physiotherapist.
If you can afford it, another option would be to have regular sessions with a personal fitness trainer at a gym. If you are able to find someone who is trained to personal trainer level two or above, they will be able to give you advice on the best exercises for you and can monitor your progress. Make sure you tell them about your condition.
Information related to managing symptoms
-
Exercises for healthy joints
Try these exercises for neck, shoulders, knees, back, hips, feet, ankles, toes, wrists, fingers and hands to manage your condition and maintain healthy joints.
-
Diet
There’s a lot of advice about diets and supplements that can help arthritis. We explain which foods are most likely to help and how to lose weight if you need to.
Understanding your condition
Having a good understanding of your condition will help you know about your treatment options and why exercise and other self-management methods are important. It will also mean you’re in a good position to get the most out of your appointments with healthcare professionals.
If you’re ever struggling with any aspects of managing your arthritis, or notice new symptoms, you should see a GP. They could also refer you to another relevant healthcare professional.
This could include a physiotherapist, who is trained to help you with exercise and help you maintain movement and function of any part of your body affected by arthritis.
Alternatively, you might benefit from seeing an occupational therapist. These are professionals who could help you overcome the difficulties that your condition might cause, by providing practical solutions.
You can be referred to physiotherapists and occupational therapists on the NHS through your GP. If you are struggling with every-day tasks at home, you may be able to get access to an occupational therapist through your local social services department.
Or you can search for private physiotherapists and occupational therapists near you through the following websites:
What will the future hold for me?
It’s difficult to say for certain how arthritis will affect you over time. In some types of arthritis symptoms can come and go.
Most people with arthritis don’t have major mobility problems, and effective treatment will help reduce the risk of joint damage, even in more severe cases.
There is plenty you can do to remain positive and proactive in all aspects of managing your arthritis and your overall health.
If you’re worried about what impact arthritis will have on your working life, it’s important to know that you have rights and options.
If you work your arthritis might mean that you need to change aspects of your job or even train for a different role.
Your employer has a duty to make sure that your arthritis doesn’t make it difficult for you to do your job, or that you’re uncomfortable at work. Having a chat with your manager about your condition, how it affects you, and how your employer might be able to help you is a useful first step to unlock the rights and support you’re entitled to by law.
Being in pain from arthritis can often lead to anxiety and depression. It’s important to tackle feelings like this, because they can affect how well you manage your condition.
Talking to your partner, relative, friend, or a doctor can really help. You might find it helpful to try something like cognitive behaviour therapy, or mindfulness. These are talking therapies that have helped people cope better with the effects of arthritis.
If you have arthritis it does have the potential to have an impact on your quality of life. However, with the right treatment, support, knowledge and approach, you will be able to live a fulfilling, happy and successful life.
The more you’re able to stay physically and socially active the more control you’ll have over your life, and the less control arthritis will have over you.