People with chronic pain need more support to manage their condition
11 May 2022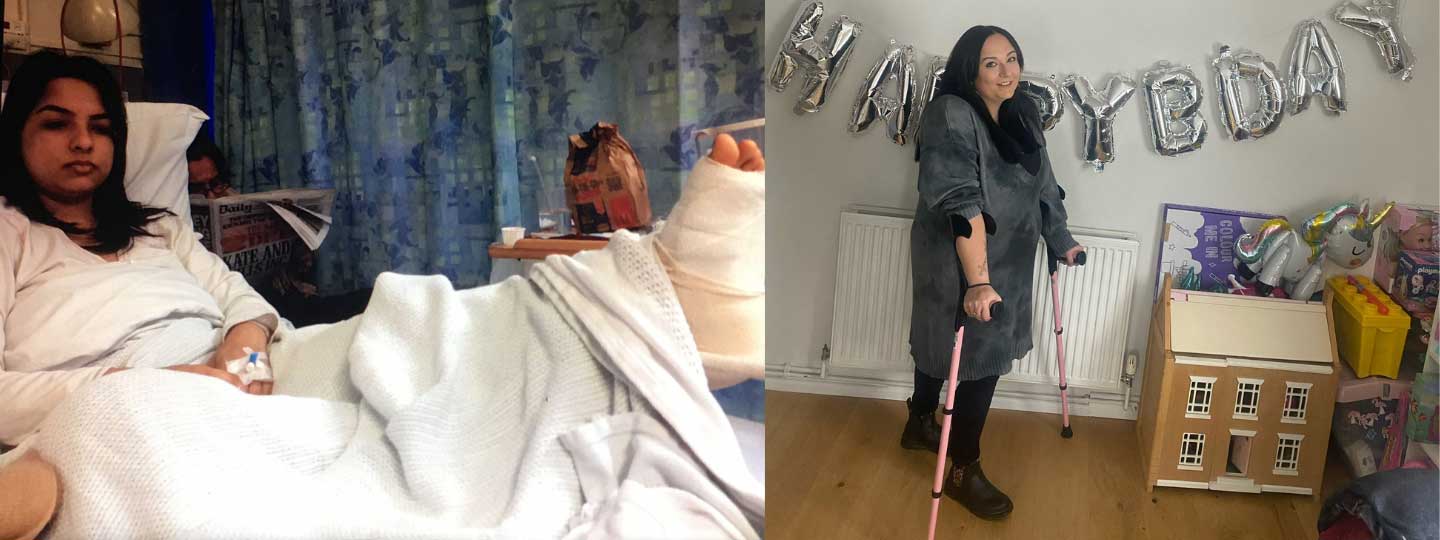
Chronic pain has been called an invisible condition. Although often devastating to the millions who have it and being one of the biggest causes of disability in the UK, to others it remains unseen.
We have worked with the BBC on new research that reveals the level and extent of people experiencing chronic pain in the UK and use of medications such as opioids.
Although chronic pain can affect anyone, including children, it is more prevalent in women, people experiencing deprivation, older people, and disproportionately affects people from some ethnic minority groups.
Millions of people in the UK have high-impact chronic pain.
People with high-impact chronic pain struggle to take part in daily activities such as self-care, family, community, and work.
Yet the current approach to treating chronic pain in the UK is poorly serving those who live with it.
An exclusive survey of over 4,000 adults aged 16-75 for BBC News, carried out by research company Ipsos, suggests that a quarter of people in the UK are living with chronic pain, and yet nearly a quarter (24%) of people with chronic pain are being prescribed opioid painkillers for their pain.
While many do get benefits from pain medication, just using medicines alone doesn’t address the issues linked to chronic pain, such as inactivity, mental health impact, or inability to work, deprivation, social exclusion and marginalisation.
The health-care system is designed to make prescribing medication the easiest form of treatment.
People with chronic pain need more than just medicines to manage their condition. Alongside medical treatments, people with chronic pain need a complex network of support that covers mental health, physical activity, community, peer-support and healthy employment.
But, unlike prescribing medicines, we don't have the infrastructure to provide people with this support on a national level.
Chronic pain can be exhausting and feel inescapable.
People living with it often face a daily struggle in which every activity - from getting moving in the morning, to washing, dressing, working, exercising, being with family and friends and even trying to sleep - is made harder or impossible.
Chronic pain can limit not just what people are able to do, but also how they feel and think. It can prevent people from fully participating in society, slowly eroding the connection to community, until they feel isolated. At its worst, chronic pain reduces and ruins lives.
Anoushka’s story
Anoushka Anand, 33, a paediatric health care assistant from London, featured in the BBC coverage.
Since 2007, Anoushka has been living with severe rheumatoid arthritis and osteoarthritis and has recently been diagnosed with moderate ankylosing spondylitis.
Due to the severity of her arthritis, she has needed multiple surgeries and lives with chronic pain every day. Anoushka is treated privately, when necessary, but is currently also receiving treatment at specialist orthopaedic NHS hospitals and has been proactive in seeking out specialists who can help. She said:
“Chronic pain has had a huge impact on my life. I have learnt thanks to my own strong desire to be able to continue in a job that I love to live with pain day to day. I take very strong opioid painkillers that helps me to manage my pain.
I also find that doing a little gentle yoga, a little tai chi, swimming, boxing and keeping fit as often as I can also helps me to manage my pain. This is because the more active I am, the less stiff my joints tend to be, which in turn helps to decrease the pain. I also enjoy keeping fit and working out and I try to get to the gym as much as possible.
“Chronic pain, although can't be seen on the outside of the body, is very real and can be very debilitating and I think this topic needs to be talked about more, so that people can better understand what it means to battle chronic pain.”
Over-medicalising chronic pain is too simplistic, and can cause more harm than good.
It is time for society and policymakers to recognise that chronic pain is a complex problem with no simple solution.
Developing a system and communities of support for people with chronic pain, and addressing the underlying causes – including deprivation, social exclusion and marginalisation – will be complex, long-term work. But continuing with an over-medicalised approach will do nothing to increase people’s chances of living well with chronic pain.
Steph’s story
Steph, 33, from Bristol, lives with fibromyalgia. She said:
“The NICE guidelines on chronic primary pain have made things difficult for me. When I first heard of the change to advice about painkillers, I thought I would have them taken away from me by my doctor, which caused anxiety.
“Medication has to play a part, and people with chronic pain need access to painkillers. I do agree with the principle of reducing painkillers. They can be addictive, but I need proper support to find treatment which I can use alongside pain meds – like psychological therapies - to give me a better quality of the life.”
What needs to happen
This is a critical moment for reform across both the health service and public health. We are calling for a fundamental re-think in how we support people with chronic pain.
We are calling for a fundamental re-think in how we support people with chronic pain. Everyone – from Government, local leaders of health and social care services, to employers, communities and the third sector - must work towards anyone in the UK living with chronic pain having access to the support they need, alongside medical treatments where appropriate, so it no longer drives millions of people into disability.
We’re here whenever you need us.
- Our free helpline 0800 5200 520 is open Monday to Friday, 9am – 6pm. If you would like to talk to someone.
- Our online community, Twitter, Facebook and Instagram communities are available and people have told us how beneficial it has been being able to connect and talk to others who are going through similar experiences.